 The development of a disease such as tuberculosis of the spinal column is a serious pathological condition of the body.
The development of a disease such as tuberculosis of the spinal column is a serious pathological condition of the body.
Tuberculous spondylitis is an infectious lesion of the bones and articular elements of the spinal column. The causative agents of the disease are the same as with the more well-known pulmonary tuberculosis, just in this case other parts of the body are affected. It also determines the specific treatment.
Bone tuberculosis causes pathological changes that affect the spongy substance of the vertebrae. Gradually, cavities form inside the bones, which are filled with connective tissue, which usually forms in the healing areas. As a result, this will also lead to the appearance of deformations. Over time, if untreated, regardless of the form of tuberculosis, serious disorders develop due to deformation of the spinal column, which can lead to consequences such as impaired mobility.
According to the area of infection, local, widespread and multiple forms of the disease are classified. In the first case, only one vertebra is affected, with a common form, pathological processes affect two or more adjacent vertebrae, with a multiple form, the disease affects the condition of several non-adjacent vertebrae.
Depending on the degree of development of bone tuberculosis, its stages are distinguished:
Stage 1 – characterized by primary osteitis, the disease is only beginning to develop;
Stage 2 – the functions of the spine are not yet impaired, but the patient has progressive spondylitis;
Stage 3 – the functions of the spine begin to be impaired;
Stage 4 – spinal functions are completely lost;
Stage 5 – characterized by the development of the consequences of tuberculous spondylitis (post-tuberculous spondylitis).
Tuberculosis infection often affects the thoracic spine. This accounts for 6-7 cases out of 10. 2-3 cases out of 10 are lesions of the lumbar region. Tuberculosis of the spine in adults is much more common than in children. Men are more susceptible to disease than women.
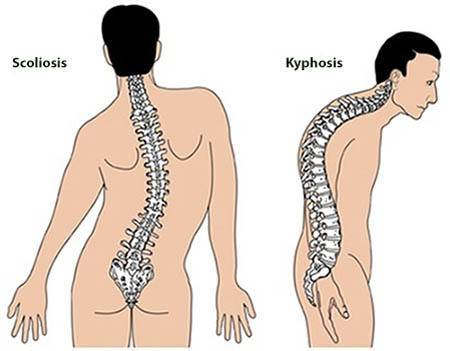
Reasons for the development.
Tuberculous damage to the spine develops due to infection in the body. It can enter the body by aerogenous, contact route or through the digestive system. Since the airborne transmission route is the most common, more often the lungs suffer from tuberculosis. Therefore, the causes of the onset of the disease are contacts with the infected. With blood flow, the infection can spread to the bone cavity or articular structures. Because of this, there is a tuberculous lesion of the spine.
The following negative factors can provoke the spread of infection to the vertebrae and joints of the spine:
– spinal injury;
– decrease in the protective functions of the body;
– smoking;
– increased load on the spine;
– subcooling;
– weakening of the body due to concomitant diseases;
– untimely or ineffective treatment of pulmonary tuberculosis.
Tuberculosis symptoms
Fever. As a rule, it is regular in nature, but the temperature is not high – 37.2-37.5.
A patient with tuberculosis quickly gets tired, often even without any reason. Often there is weakness throughout the body. Sometimes there is increased irritability.
With the defeat of one vertebra or joint, the patient feels pains in the spine, which are manifested slightly. It is difficult to determine their location. Usually, pain appears after exertion, for example, in the evening after a working day. After rest, the pains disappear, but from time to time appear again.
With the spread of infection, painful sensations become more pronounced and pronounced. Over time, they occur even when there are no loads on the spine. Drugs with anti-inflammatory and analgesic effects will not be effective in this case.
Limited movement develops. It is rather difficult to turn or bend to the patient. Strong and intense pains appear. The back muscles are painful, especially when pressed. They are constantly tense. Over time, body temperature becomes higher – 38-40 degrees. In the area of the affected vertebra, a small tubercle can be felt, and if the lesion is extensive, then a whole hump appears, which will become more and more. The body of patients with severe tuberculosis that affects the spine is deformed, becomes curved.
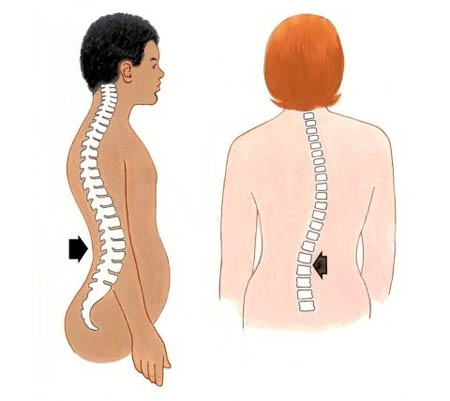
Diagnosis of spinal tuberculosis
To confirm tubspondylitis, it is necessary to conduct laboratory diagnostics: a general blood test, a general urinalysis, a biochemical blood test, an X-ray examination of the spine (including methods such as MRI and CT of the spine). Immunological tests help the diagnosis: Mantoux test and Diaskintest. It is also necessary to conduct a bacteriological study of the discharge from the tinea and fistula on the MBT and the GeneXpert study. Patients with suspected tubspondylitis consult a traumatologist and phthiso-orthopedist to confirm the diagnosis.
In cases of infection affecting only the spine, the evaluation is not simple, requiring bone and disc biopsy to confirm the diagnosis and enable the start of treatment. Even with biopsies, where the material taken from the affected region is analyzed microscopically and used for the cultivation of the bacteria, the diagnosis in some cases may be uncertain. Fortunately, nowadays we can count on tests applicable to biopsies in which the DNA of tuberculosis bacteria is analyzed, and the diagnosis can be made, even if a minimum amount of material is available.
Treatment
Treatment of the disease can be quite long and complicated. The patient needs hospitalization in a specialized hospital.
Most of the cases, mainly those diagnosed in the initial phase, the treatment can be done conservatively, using continuous vests, and using a combination of medications, used for periods usually longer than six months. In some cases, when the bacterium causes great bone and joint destruction of the spine, causing severe deformity, or when there are abscesses or compression of nervous structures, surgical treatment is necessary. Generally, these cases should be followed up by a specialist with more experience in the area of spine surgery, as they may require complex and major surgeries for the reconstruction of the structures destroyed by the disease.
